 Examination of the fellow eye should be mandatory as there is a high incidence of bilateral pathology. Round hole detachments are slowly evolving detachments with attached vitreous gel in young, predominantly female myopes. In all, 99% detachments were successfully reattached with a single procedure. A total of 100 detachments were repaired with cryotherapy and scleral buckling, eight with cryotherapy alone, and one with laser retinopexy. Detachments were predominantly shallow (93%) and slow in progression (17%). In all, 45% patients had bilateral pathology, of which 33% had ‘mirror image’ distribution. The posterior hyaloid membrane remained attached in 95 eyes (86%). The mean age for patients was 34 years with a marked female preponderance (64%) and myopia (83%). Analysis of patient age, sex, refraction, preoperative visual acuity, presented symptoms, position and extent of detachment, number and distribution of holes present, posterior hyaloid membrane status, surgical management, outcome of surgery, and postoperative visual acuity were studied. In all, 110 retinal detachments from 96 consecutive patients with retinal detachment secondary to round retinal holes were studied. This study characterises the features, surgical outcome, and incidence of bilateral involvement of detachment associated with round retinal holes Methods 
Retinal detachment without PVD is usually associated with either retinal dialysis or round retinal holes. If you notice any sudden change to your vision, pain, redness, or unusual discharge you must contact The Retina Clinic London.The majority of rhegmatogenous retinal detachments result from pathological posterior vitreous detachment (PVD) and secondary horseshoe or giant retinal tears. Prof Stanga will be reviewing you frequently to ensure the eye is healing well. This can lead to complete and permanent loss of vision, if not treated. Infection –This occurs very rarely and would require urgent treatment. If a cataract is already present it can be removed at the same time. High pressure – If the pressure in the eye goes very high for a short period of time or goes slightly up for a prolonged period of time the optic nerve can be damaged resulting in partial or complete and permanent loss of vision.Ĭataract formation – It is almost certain that a cataract will develop within 36 months of this operation. However, this can usually be repaired with a further procedure.īleeding – This occurs very rarely and could cause complete loss of vision if severe enough. Retinal detachment – The retina can detach from the back of the eye resulting in complete vision loss. It is, therefore, possible that the surgery may need to be repeated. The hole fails to close – This can lead to worse vision than before surgery. Stanga will confirm this with you at your consultation. The typical waiting time for this is around 4-6 weeks, however, Prof. You must not fly or travel at high altitude or drive until the bubble has been sufficiently absorbed. Early diagnosis is very important as final vision quality can be dependent on how long the hole has been present and its size, amongst other factors. Vision can take several months to improve to its maximum potential. As a result, your vision will start to improve. Approximately 7-15 days after the treatment, the bubble starts to shrink and will be replaced by the natural fluid produced by your eye. Initially, the vision in your eye will be very poor. 
This allows for the bubble of air or gas and the macular hole to maintain full contact. To ensure the macula has the best chance of healing you may be asked to assume a face-down position (known as posturing) for 24 hours after surgery. 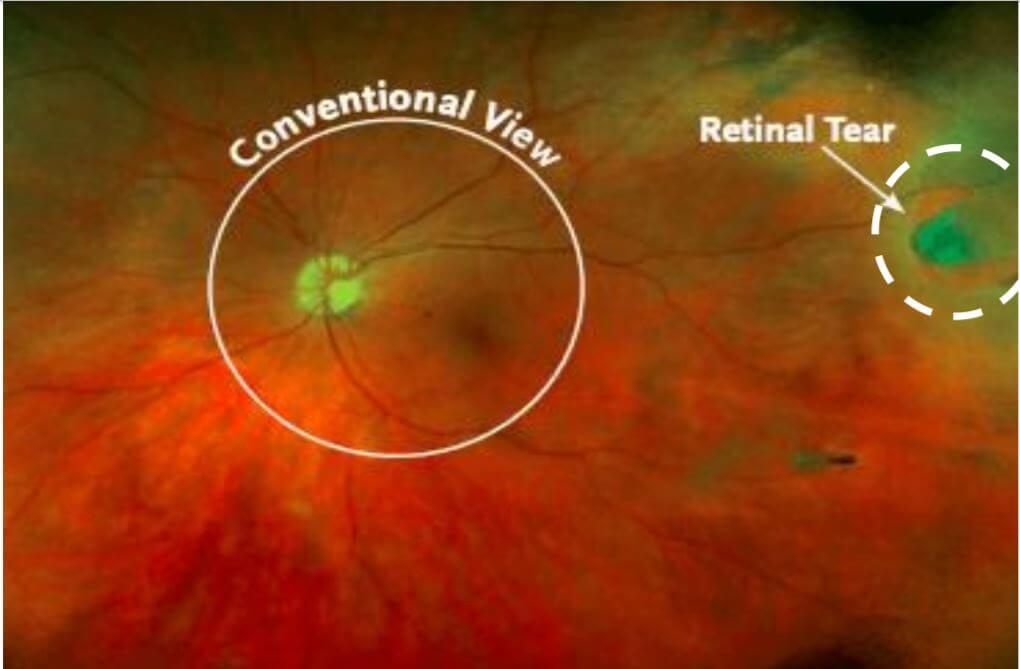
Macula Hole – Post-treatment (Figure 2 shows macular hole post-treatment) Follow-Up After Treatment An air or gas bubble is injected to encourage the macular hole to close. The most common course of treatment is to have an operation called a Vitrectomy.ĭuring this procedure, the gel inside the eye is removed, and the retinal tissue on the surface of the macula is peeled and placed into the hole to fill the gap. Macula Hole – Pre-treatment (Figure 1 above shoes a macular hole pre-treatment) What Is the Treatment for A Macular Hole? It pulls on the retina and macula, in some patients, causing a hole. As we age, the vitreous humour (the gel inside the eye) starts to liquefy and collapse. Macular holes are commonly found in patients between 60 and 75 years of age and are more common in females. The condition does not lead to a total loss of vision and is not painful. This hole can cause the central part of your vision to be missing, distorted, or blurred. A macular hole is a small opening in the very centre of the area of the retina called the macula. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
